
For the first time in its history, the 73rd Annual Meeting of the American Academy of Neurology (AAN) – the world’s premier neurology meeting – was held in a fully virtual format from April 17th to 22nd 2021
Welcome to AAN 2021

James Stevens, AAN President
The 2021 virtual AAN annual meeting was centred around a rich educational and scientific programme including over 90 expert-led educational courses, more than 2000 scientific abstracts and seven key plenary sessions featuring leaders in neurology.
AAN President James Stevens, Fort Wayne, USA, began this key plenary session with presentation of the President’s Award followed by the Presidential Lecture entitled: ‘Disruption: How to Pivot from Uncertainty to Success - the AAN Story.’ Dr Stevens proposed a focused five-pronged approach to navigating crises such as COVID-19.

Five-pronged approach to navigating crises such as COVID-19.
“What a year it has been - unprecedented does not even begin to describe what we have all been through. We’ve faced uncertainty, exhaustion and challenge but we are emerging stronger, resilient and prepared to face our new future. ”
President James Stevens, Fort Wayne, USA

Orly Avitzur, AAN President-Elect
The 2021 virtual AAN annual meeting was centred around a rich educational and scientific programme including over 90 expert-led educational courses, more than 2000 scientific abstracts and seven key plenary sessions featuring leaders in neurology.
There then followed a brief welcome address by AAN President-Elect Orly Avitzur, Tarrytown, USA, who will be charged with leading the academy over the next two years. As we enter the recovery phase of the pandemic, Dr Avitzur outlined some exciting AAN programmes for the future including an increasing focus on hybrid educational and scientific meetings, studies to support telemedicine and an expanded emphasis on well-being.
COVID-19
Neurological perspectives on COVID-19

For the first time in AAN history, the 2021 Hot Topics Plenary Session focused entirely on a single issue - the global COVID-19 pandemic. The plenary began with a Q&A session involving Walter Koroshetz, Bethesda, USA, and Anthony Fauci, Bethesda, USA, leading figures who have been at the forefront of the recent public health crisis. A range of topics were discussed including vaccine safety, viral transmission in vaccinated individuals and the promise of new targeted antiviral therapies. Dr Fauci described the extreme variability in COVID-19, with cases ranging from asymptomatic infection to severe disease resulting in intensive care unit (ICU) ventilation and death, as a ‘pathogenic mystery’ not seen in any other infectious disease. From a neurology perspective, Dr Koroshetz highlighted a key role for neurologists in dealing with post-acute sequelae of SARS-CoV-1 infection (PASC) and suggested that, in the future, mRNA vaccine technology developed during the pandemic may be used to eradicate neurologically relevant infectious pathogens, most notably Epstein Barr virus.
“We know very little about the biological underpinnings of PASC but we do know that it’s not a minor problem…I think that neurologists have to play a really important role in trying to get the bottom of this.”
Walter Koroshetz, Bethesda, USA
Four speakers then summarised recent COVID-19-related research findings and discussed their clinical implications. Sherry Chou, Pittsburgh, USA, presented the first report from the global cohort study on COVID-19 acute neurological manifestations, a large multicentre study involving 28 centres from 13 countries which included cohorts of hospitalised COVID-19 patients from the both ENERGY Registry (n=214) and the GCS-NeuroCOVID consortia (n=3055). Acute encephalopathy (50%), coma (17%) and stroke (3.1%) were found to be the most prevalent acute neurological manifestations in hospitalised COVID-19 patients. Neurological signs/syndromes dramatically raised the risk of death, with a x5.5-fold increase in mortality in patients developing the most common complication of acute encephalopathy compared to COVID-19 hospitalised patients without neurological manifestations. Key risk factors for developing acute neurological complications with COVID-19 included older age, male sex, white race and pre-existing neurological disorders, which raised the risk by 2.2 fold.

Risk of mortality in COVID-19 patients with neurological symptoms during acute hospitalisation vs. those without
The global pandemic has shone a spotlight on health disparities in black, Asian and minority ethnic (BAME) populations, said Nicte Mejiam, Boston, USA, with greater COVID-19 related mortality in these patients driven by subpar access to critical and specialty care and therapeutics, as well as differential goals of care. Moving forward, Dr Mejiam suggested three key initiatives to help dismantle this structural racism and promote justice: a single payer national health programme, telemedicine and medical licensure reform and a rebuilding of the public health infrastructure.
There are increasing literature and anecdotal reports of neurological complications after recovery from acute COVID-19 including a wide spectrum of cognitive, mood, sensory, motor, autonomic and headache symptoms. Current understanding and clinical experience of these neurological syndromes post-acute COVID-19 were explored by Serena Spudich, New Haven, USA. Preliminary research findings suggest that persistent neuroinflammation and regional cerebral hypometabolism may play a potential role in pathogenesis. Future work will seek to identity laboratory biomarkers associated with post-COVID-19 neurological syndromes and, most importantly, identify ways to best manage and resolve these disorders.
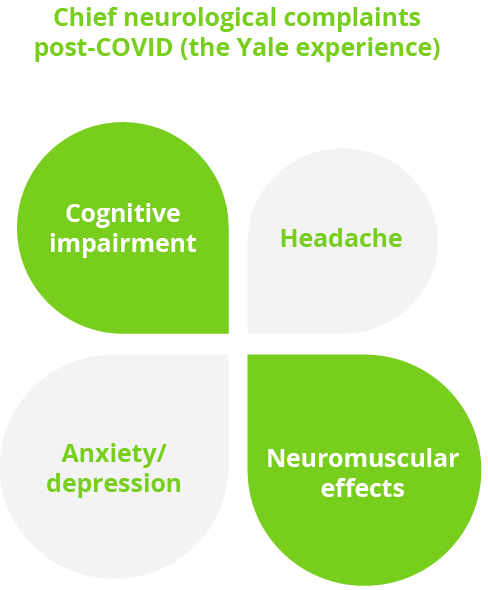
The Yale experience of chief neurological complaints post-COVID
Igor Koralnik, Chicago, USA, discussed COVID-19 vaccines and the immunological response from a neurologist’s perspective, highlighting issues around the reliability of serological testing, rapid decay of antibodies in people with mild COVID-19 disease and cases of reinfection. Dr Koralnik referenced a specific study of non-hospitalised COVID-19 ‘long haulers’ carried out at his Neuro-COVID-19 clinic which showed T-cell responses to SARS-CoV-2 proteins, with even some RT-PCR or AB-negative patients having T-cells capable of recognising SARS-CoV-2 proteins on interferon-y ELISPOT. Important unanswered questions include the neurological side effects of vaccines and their effect on PASC.
Management of neurological complications of COVID-19

An educational course summarised current management of acute and chronic neurological complications of COVID-19. Kenneth Tyler, Boulder, USA, reviewed the acute neurology of COVID-19 and described four different routes by which neurological manifestations can arise. An increasing body of evidence from epidemiological studies has confirmed encephalopathy and acute cerebrovascular disease (most commonly ischaemic stroke) as the major neurological complications of systemic COVID-19 disease.
Cases have also been reported of direct SARS-CoV-2 CNS invasion which can produce syndromes of encephalitis/meningoencephalitis and myelitis. There are several categories of COVID-19 encephalopathy and encephalitis, highlighted Dr Tyler, each with different clinical and laboratory features. Among the post-infectious, immune-mediated complications of COVID-19, Guillain-Barre syndrome (GBS) and acute disseminated encephalomyelitis (ADEM) were most common. The majority of patients (70%, n=42) affected by GBS had classical sensorimotor GBS, but motor variants (~7%, n=4) and Miller Fisher syndrome (~12%, n=7) were also seen. Other reported neurological manifestations of COVID-19 due to PNS/muscle involvement included disorders of smell and taste (anosmia and dysgeusia) and myopathy (possibly due to a type 1 interferonopathy). Dr Tyler pointed out that almost all of these neuro-COVID syndromes have also been described in infected children, albeit more rarely.
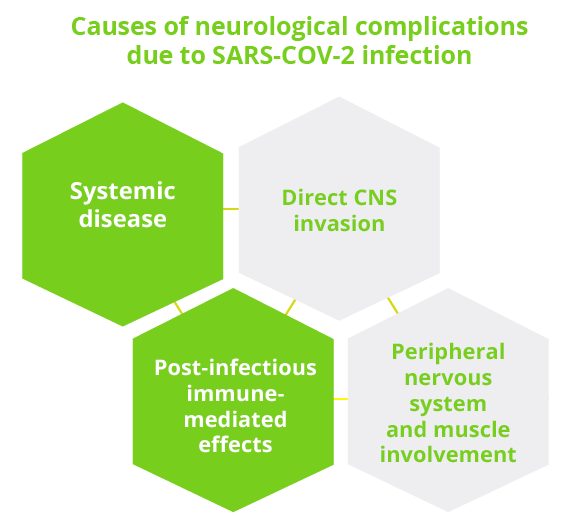
Causes of neurological complications due to SARS-CoV-2 infection
“The mechanism (of smell and taste disorders with COVID-19) remains controversial but looks like it may be due to inflammation and injury of nasal epithelial cells that surround the olfactory neurons.”
Kenneth Tyler, Boulder, USA

Long-term neurological complications of COVID-19 were addressed by Igor J. Koralnik, Chicago, USA, who reviewed key global studies showing that the same neurological manifestations of COVID-19 occur worldwide, albeit at a higher frequency in the US (82%) and Europe (57%) as compared with China (36%). Encephalopathy was found to be the major contributor to poor outcomes and mortality irrespective of geography. Dr Koralnik then presented results from a prospective study of 100 non-hospitalised COVID-19 ‘long haulers’ conducted at the Northwestern Memorial Hospital Neuro-COVID-19 clinic. The study revealed ‘long haulers’ were affected by prominent and persistent brain fog and fatigue, as well as impaired attention and working memory, accompanied by reduced quality of life in areas of cognition and fatigue. Among patients affected by long COVID, there was a high female to male ratio and prevalence of pre-existing autoimmune disease, consistent with a post-infectious autoimmune aetiology. Time to onset was not a good predictor of recovery in this population, noted Dr Koralnik, with patients typically following their own individual trajectory.
“Based on reports from all over the world it seems like millions of people are affected by long COVID syndrome which means there will be a significant impact on the workforce.”
Igor Koralnik, Chicago, USA
Closing Remarks

Hailing this year’s annual meeting as ‘ANN excellence delivered unconventionally’ outgoing President Dr Stevens closed the congress by handing the reins of leadership to the new ANN President Dr Avitzur with the passing of the gavel. Dr Avitzur expressed her hope for an optimistic future with next year’s AAN meeting, due to take place in Seattle, Washington, between the 2nd and 8th April 2022, providing the opportunity for members to come back together again in person.
©Springer Healthcare 2021. This content has been independently selected and developed by Springer Healthcare and licensed by Roche for Medically. The topics covered are based on therapeutic areas specified by Roche. This content is not intended for use by healthcare professionals in the UK, US or Australia. Inclusion or exclusion of any product does not imply its use is either advocated or rejected. Use of trade names is for product identification only and does not imply endorsement. Opinions expressed do not reflect the views of Springer Healthcare. Springer Healthcare assumes no responsibility for any injury or damage to persons or property arising out of, or related to, any use of the material or to any errors or omissions. Please consult the latest prescribing information from the manufacturer for any products mentioned in this material.